Otitis or ear infections are one of the most common ailments affecting children and adults alike. Generally, ear infections are referred to as otitis, a term designating both an infection and an inflammation of the ear.
They can affect the outer ear, the middle ear or the inner ear and treatment depends on the severity and type of infection. If left untreated, ear infections can lead to hearing loss.
Infections of the middle ear are simply referred to as ear infections, earache, otitis media, acute otitis media or chronic otitis media. Infections of the outer ear are called ear canal infections, swimmer’s ear or otitis externa, but also earache.
Infections of the internal ear are referred to as labyrinthis or otitis interna. Generally, ear infections are caused by either bacteria or viruses and can be acute or chronic.
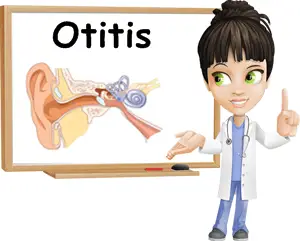
What is an acute ear infection?
Acute ear infections are very painful, but short in duration and may not even require antibiotic treatment, depending on the cause.
What are chronic ear infections?
Chronic ear infections are generally not as painful, but tend to recur. They are more dangerous because, if not treated properly, they may lead to permanent ear damage and even hearing loss. Ear infections are one of the most common types of infections in both children and adults.
Why do ear infections (otitis) hurt so badly?
Ear infections are caused by either bacteria or viruses. These pathogens cause damage at the site of the infection by attacking our body. As a result, inflammation occurs. And it’s inflammation that causes the actual pain in ear infections.
In many cases, fluid also builds up inside the ear, creating pressure and adding to the pain. Depending on the area affected, ear infections may have different causes, exhibit different symptoms and even require different treatments.
Ear infection symptoms
Signs and symptoms of an otitis externa (external ear infection) can include:
1) Ear pain. This is the most telling symptoms and often the only one directly associated with external ear infections.
2) Swelling of the outer part of the ear.
3) Itching.
4) Discharge.
Signs and symptoms of otitis media (middle ear infections) can include:
1) Ear pain.
2) Fever (especially in children).
3) Irritability.
4) Ear discharge.
5) Cough.
6) Runny nose.
The cough and runny nose symptoms that may accompany middle otitis are actually symptoms of a preceding respiratory tract infection that might have favored the ear infection.
Signs and symptoms of otitis interna (inner ear infection) can include:
1) Vertigo, a form of dizziness, and symptoms associated with it: nausea, vomiting, problems walking, anxiety, sweating and an overall feeling of unwell.
2) Ringing ears or tinnitus.
3) Hearing loss.
Why do ear infections cause dizziness?
The vestibular system is what provides us with our sense of balance and helps us coordinate our movements. This vestibular system is situated in the inner ear, in an area called labyrinth (hence the names labyrinthitis and vestibular neuronitis for otitis interna). When we get otitis interna, an inflammation of the inner ear, the vestibular system is affected which leads to dizziness.
Ear infection causes
External ear infections (otitis externa) can be caused by:
1) Water trapped in the ear canal (after showering, swimming).
2) Bacteria or fungi introduced in the ear canal via dirty hands, dirty water or cottons swabs, etc.
3) Cleaning ears with cotton swabs, fingernails, keys, pen caps, needles, hairpins, pencils which may hurt the ear and provided an adequate medium for bacteria to flourish.
4) Injury to the ear, including ear piercings.
Middle ear infections (otitis media) can be caused by:
1) Allergies.
2) Viral upper respiratory tract infections (common cold, rhinitis, pharyngitis, laryngitis).
3) Streptococcal pharyngitis causing sore throat, fever, red tonsils, swollen neck lymph nodes, etc.
4) Excess phlegm or mucous reaching the middle ear and causing a bacterial infection.
5) Cigarette smoke or other irritants.
Eustachian tube problems favor the accumulation of fluid in the middle ear and existing respiratory tract infections can lead to bacterial infections and otitis media.
Internal ear infections (otitis interna) can be caused by:
1) Viral infections (example: Herpes simplex type 1).
2) Bacterial infections.
3) Injury to the head or ear area.
4) Allergies.
5) Medication side effects.
6) Stress.
It has been observed that internal ear infections are often preceded by an upper respiratory tract infection such as the common cold or a flu.
Why do ear infections, also known as otitis, occur?
Ear infections of the middle and inner ear (otitis media and otitis interna) generally occur following an upper respiratory tract infection, as a result of either a virus or a bacteria, rarely a fungus.
If there isn’t a preceding respiratory tract infection, otitis media and otitis interna may be a result of poor hygiene.
Many people are in the habit of scratching their ears or cleaning them of earwax with their fingernails or various objects such as pencils, hairpins, etc.
What people don’t know is that if they are not careful, any object they may introduce inside their ear may hurt it as it is a highly sensitive organ.
Hurting the delicate skin creates the perfect occasion for bacteria or viruses to infiltrate and create an infection. Even cotton swabs can be full of bacteria if they are handled with dirty hands, hence one of the reasons why otitis is so common.
Moreover, constantly taking out every little particle of earwax can favor otitis because earwax, in small amounts, acts as a protective barrier, preventing the access of bacteria inside the ear.
Otitis of the external ear is a particular case. While swimming in the ocean or in a not so clean swimming pool can cause bacteria to accumulate and cause an infection, even clean water left inside the ear for some time can lead to external otitis. This is because prolonged humidity or constant exposure to water disrupts a fragile balance at the level of the ear, favoring bacterial infections. Scratching the ear canal with one’s fingernails or a pen cap, hairpin or other sharp object can hurt the skin and allow for an infection to develop.
What to do about it
Treatment options vary from case to case and may depend on the severity of the infection, age of the sufferer, whether or not the infection has recurred and so on.
A visit to the doctor is in order for a professional diagnosis and a personalized treatment approach. While some people may require antibiotic treatment in the form of ear drops, especially for bacterial infections, others are recommended to simply manage symptoms and avoid risk factors to allow for the infection to clear itself.
In some cases, antibiotics taken without a doctor’s consent may cause the infection to aggravate.
In any case, it is important to see a healthcare professional because, if not treated properly, otitis can lead to serious complications that may result in the perforation of the ear drum, hearing loss, bacterial meningitis, etc.
People suffering from internal otitis might require physical therapy exercises or certain medication to help them with the dizziness symptoms. If the cause if allergies, antihistamine medication may be prescribed.
Here are a few important tips for preventing otitis:
1) Wash your hands frequently. This way, even when we accidentally scratch our ears, chances our hands are already clean and we don’t risk an infection. Nevertheless, it is always best to use a sterilized cotton swab to help keep our ears clean.
2) Avoid smoking. Both first-hand smoke and second-hand smoke. Tobacco smoke is one of the most common irritants which can cause ear problems. As uncanny as it may seem, it is best to avoid cigarette smoke if you wish to keep healthy.
3) Pay attention where you swim. If you experience frequent otitis after using a public swimming pool or swimming in the ocean or sea, then it might be best to choose a private swimming pool you know for certain meets certain cleanliness standards. If humidity or exposure to water itself is the problem, you might consider changing hobbies for a while until your ear infection clears up.
4) Keep ears dry. It is important to keep our ear dry in order to prevent ear infections. So remember to dry your ears after getting out of the shower, swimming pool, etc. If you are not so great with cotton swabs and feel they are too intrusive, here is a tip from an otolaryngologist that I have found very useful: lean the head on one side and use the edge of a clean towel to gently dab the ear dry. Do the same for the other ear. I find this very useful and it saves me the trouble of having to use cotton swabs as I almost always hurt my ears with them.
5) Avoid daycare. If your child has developed otitis, it might be best to keep him or her out of day care until he or she is fully recovered. If there are cases of otitis within your child’s daycare group, it may be better keeping your child out of daycare until the other children are fully recovered.
