Blood cholesterol is an important indicator of cardiovascular health. Maintaining optimal levels of both LDL and HDL cholesterol is pivotal for preventing cardiovascular disease in all its forms, from atherosclerosis to heart attack and stroke. But there is more to cholesterol than just good and bad because, believe it or not, this fat molecule fulfills some rather astonishing functions within our body.
From digestion to hormone synthesis and vitamin absorption, cholesterol is essential for keeping us alive and in good health.
Having both too high and too low blood levels is dangerous for us. While addressing modifiable factors such as diet and exercise can have a deep positive impact on our health and lower high cholesterol levels, it turns out that genetics also plays a crucial part in how high our cholesterol may end up being.

What is blood cholesterol?
Also referred to simply as cholesterol, blood cholesterol refers to how much of a lipid (fat) called cholesterol we have per deciliter of blood. Cholesterol is basically a type of organic lipid (fat) molecule known as sterol. While we measure its blood levels, this fat molecule is present in more places than just our bloodstream. Actually, cholesterol molecules help make up cell membranes by ensuring their integrity, mobility and viability.
Dietary vs blood cholesterol
Difference between blood cholesterol and dietary cholesterol
Both are essentially the same thing, a lipid, the difference being the first is found in the bloodstream, while the second in food. Animal products such as meat, eggs, milk, dairy, fish and seafood in general all have cholesterol. Plants too have a form of cholesterol called phytosterol (or plant sterols) which our body uses in similar ways to cholesterol.
The reason why consuming more fruits and vegetables than animal products is said to lower cholesterol levels is because the phytosterols from plants, being so similar to cholesterol, compete with the latter for absorption at the intestinal level.
But, as new research reveals, cholesterol from food doesn’t play such a big role in regulating blood cholesterol levels and affecting cardiovascular health, as previously thought. It has been shown that sugars and fats in general, both rich in calories, are more likely to negatively impact cardiovascular disease.
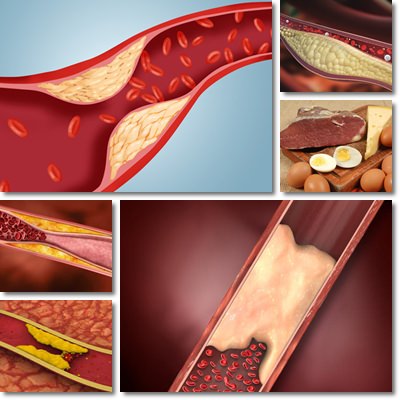
Where is cholesterol found?
Contrary to popular belief, cholesterol doesn’t come from dietary sources alone. Our body makes its own cholesterol and synthesizes it in the liver, intestinal tract, adrenal glands (above our kidneys).
Up to 25% of our body’s cholesterol production comes from the liver. The cholesterol our liver produces makes up bile which aids in digestion.
What is interesting is that our body regulates its production of cholesterol depending on how much cholesterol from animal products we take in when eating. Even more interesting is the fact that at the end of the digestion process our body takes back some cholesterol to recycle it for further use. This is done with the help of the small intestine which absorbs cholesterol and sends it back to the bloodstream.
How is cholesterol made?
Well, our body takes in all that we are feeding it and makes cholesterol out of it, mostly with the help of our liver. The liver can produce up to 1,000 mg of cholesterol a day, depending on how much our body needs.
The most amazing thing is that our body knows how much cholesterol cells need and regulates it production accordingly as well as depending on how much of what it needs we supply through diet.
HDL vs LDL
There are basically two main types of cholesterol of relevant to cardiovascular health:
1) HDL (high-density lipoprotein) cholesterol or good cholesterol. Why is HDL cholesterol the healthy type? Because HDL cholesterol is sent by the liver to gather the surplus LDL cholesterol from the body and bring it back to be recycled. Because of its function, HDL cholesterol is thought to help prevent plaque buildup, atherosclerosis and artery blockages that may lead to heart attack and stroke.
2) LDL (low-density lipoprotein) cholesterol or bad cholesterol. LDL cholesterol is generally present in greater amounts in the blood than HDL (good) cholesterol. And it is this surplus circulating freely in the bloodstream that tends to stick to artery walls and, in time, block blood flow partially or even completely. More specifically, high LDL cholesterol levels will, in time, lead to stiffer blood vessels, blood flow obstruction and ultimately stroke and heart attack.
What is the difference between low-density and high-density lipoproteins?
Cholesterol (which is a fat molecule and thus not soluble in water or blood) is carried into the bloodstream with the help of a special protein which allows it to move through the blood and go wherever needed, hence the name lipoprotein.
Low-density or high-density refers to the quality of the protein that binds to the fatty molecules. Low-density lipoproteins, for example, are the type most likely to stick onto artery walls and contribute to plaque buildup and subsequent cardiovascular problems such as atherosclerosis, high blood pressure, heart attack or stroke.
What is normal cholesterol level?
Together, LDL and HDL cholesterol as well as triglycerides (another type of blood fat) make up total cholesterol. Too high or even too low cholesterol levels can engender health problems. Blood cholesterol is measured in milligrams per deciliter (mg per dL).
Normal levels should be:
(Total cholesterol) Less than 200 mg/dL
(LDL cholesterol) Less than 100 mg/dL
(HDL cholesterol) Over 60 mg/dL
(Triglycerides) Less than 150 mg/dL
Bad dietary habits such as eating too much processed foods, junk food, packaged foods, all rich in saturated fats, and having a high intake of animal products such as butter, cheese, milk, meats or eggs can up LDL cholesterol levels and lower HDL cholesterol to unhealthy levels.
Lack of exercise, even smoking have similarly negative effects on blood cholesterol and cardiovascular health.
Moderate exercising, mostly keeping active, maintaining a healthy weight and increasing our intake of fresh fruits and vegetables while reducing animal products intake can help regulate LDL-HDL ratio and bring cholesterol to healthy levels.
Nevertheless, as more recent research appears to suggest, genetics plays an equally important part in determining our cholesterol levels and cardiovascular disease risks.
This has to do with the amount of cholesterol our body produces and uses. For example, although we may eat right, our body has its own production target and may produce more cholesterol than needed which puts us at risk for high cholesterol levels and cardiovascular disease. This, of course, may prove manageable through proper diet and exercise.
Keep in mind that cardiovascular disease is often the result of the damage produced by various risk factors and takes time to develop. Having your total cholesterol and LDL cholesterol levels checked regularly, especially if you have a family history of hypercholesterolemia, can provide you with precious knowledge and allow you to make healthy changes before bad cholesterol or any other risk factor may cause any serious damage.
